February 16, 2022
Dr Rawiri Taonui COVID Omicron Māori | Rising cases, widening tamariki vaccination gap, home isolation risk


Current Situation
Kua tomo te urutā ki roto i te whare Māori. Omicron arrived in New Zealand on 7 December.
• Ten weeks later, Omicron has set multiple new case records as high as 981 yesterday.
• The total number of community cases reached 17,354 today.
• Active cases in the community and MIQ have passed 5,600.
Taking an average three-day incubation period, current daily cases are a snapshot of infections last weekend. On that basis, the current number of new cases in the community is five times higher already.
Weekly Cases by Ethnicity
• Māori cases dominated weekly Delta case numbers from late September through to December.
• After a massive vaccination and leadership effort from Whānau Ora, iwi, and other Māori providers, Māori cases fell during December at a faster rate than for other ethnicities.
• By mid-January, weekly Māori cases were lower than for Pākehā and by the end of the month lower than weekly cases in the Asian community.
• As Omicron numbers steadily increased through late January and early February, Māori case numbers have remained low compared to Pākehā, Asian and Pacific
• Cases in the Asian and Pākehā community dominated the last week of January and the first week of February.
• The last 11 days have seen a dramatic rise in cases in the Pacific community with over 1,450 cases reported in the last week to 14 February.
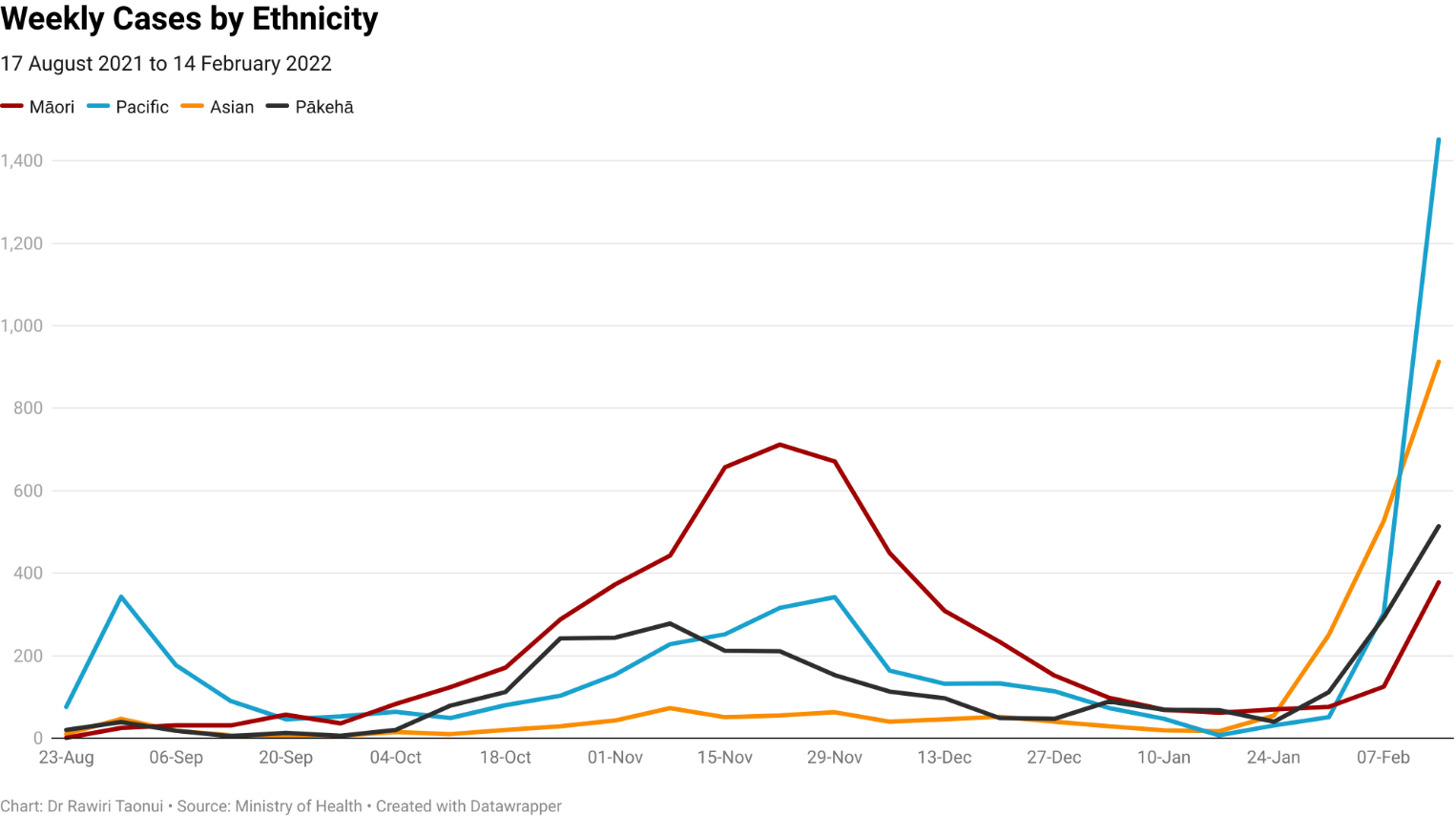
Photo Supplied
Rise in Māori Cases
Māori cases numbers remain low relative to non-Māori.
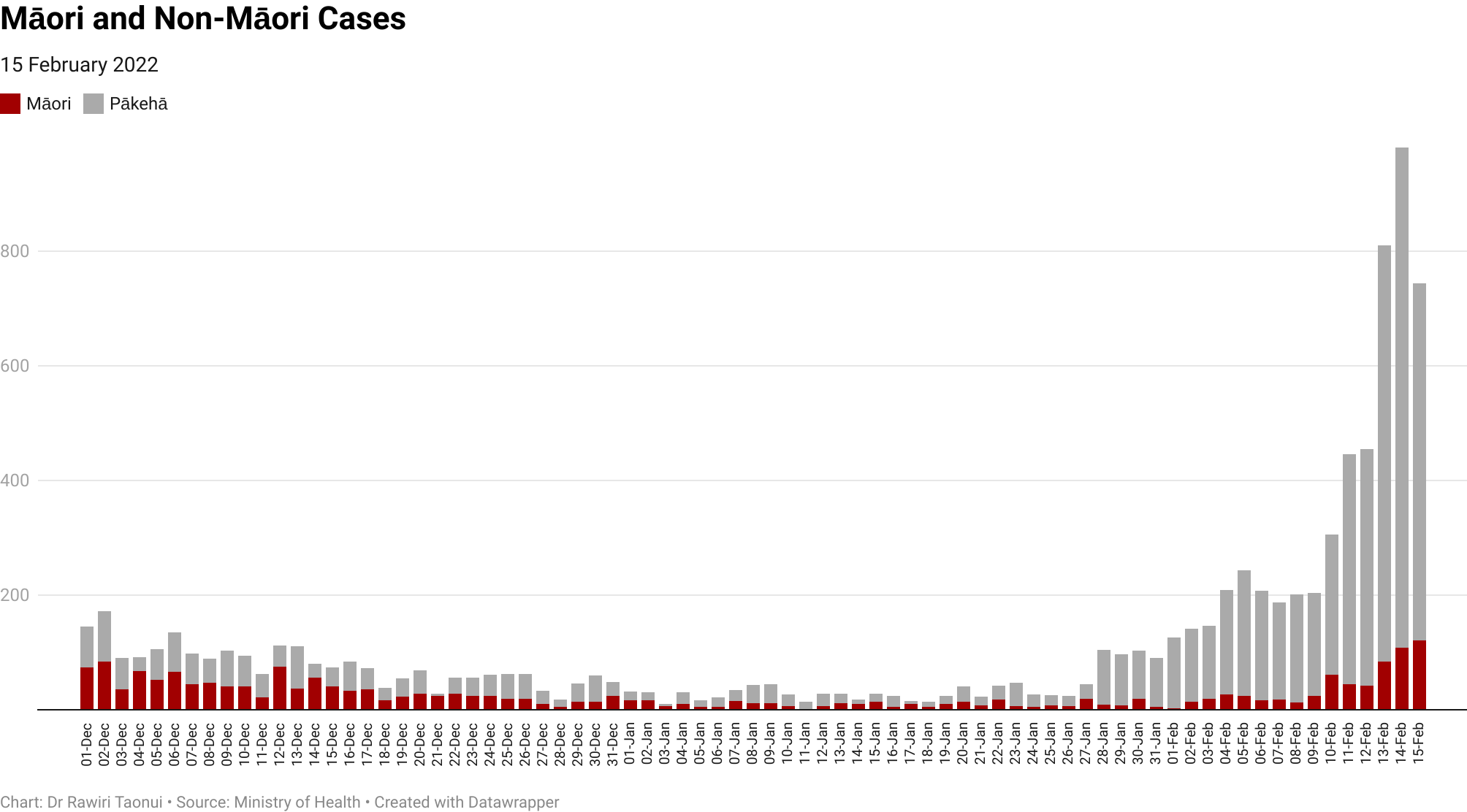
Photo Supplied
Lower Māori cases during January and early February gave Māori a window of opportunity to plan and prepare for the inevitable tsunami of Omicron cases and the government time to establish a Māori Omicron Strategy supporting home isolation.
With 313 new cases in the Māori community over the last three days, the highest since the end of November last year, that window is now closing.
And actual numbers are much higher. Several factors indicate this, including the incubation period (as above), high numbers of asymptomatic cases, and lower testing because of our lower socio-economic profile and geographic spread across urban-rural regions, and strong pockets of resistance.
New Vectors
Two vectors operating at present will steepen the rapid rise in Māori cases.
One route for Omicron into the Māori community is via the exceedingly high number of cases in Auckland particularly the Manukau DHB where there are over 2,600 cases.
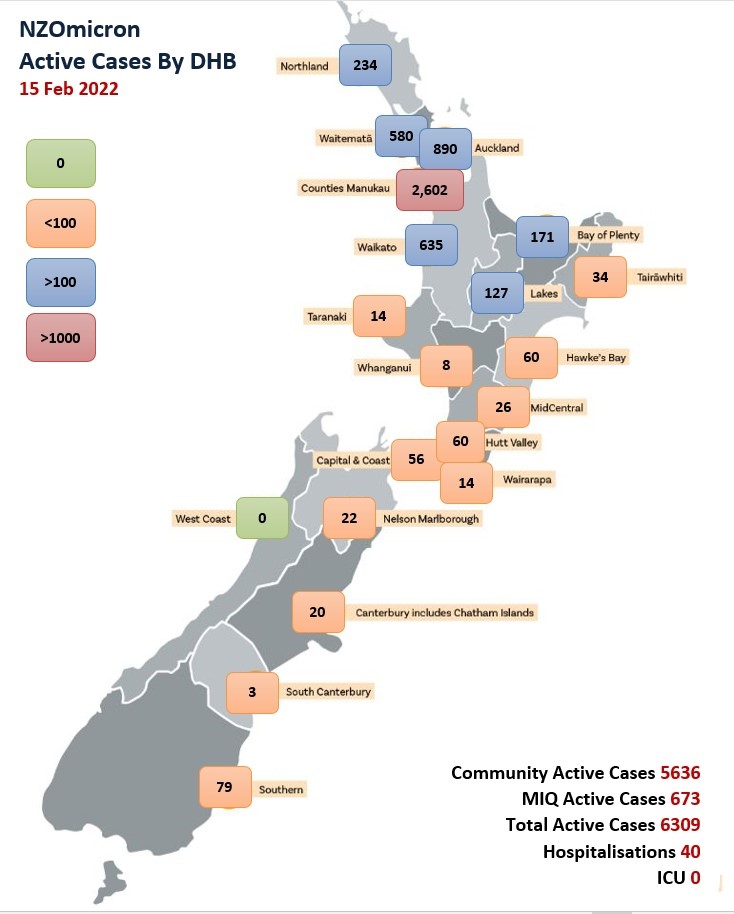
Photo Supplied
The second is our tamariki returning to schools and mixing in proximity with other children creating a greater risk of transferring infections into whānau Māori.
Kaumātua
We need to assume that Omicron is everywhere and be especially cautious with our kaumātua and whānau with underlying health conditions or those living in Auckland where the bulk of cases are.
People who are older or have underlying illnesses are more vulnerable to a serious outcome. Where possible, they need to start taking precautions to limit their range of social contacts.
If you are kaumātua or have health conditions and you are out interacting with people indoors you need to be wearing a mask the whole time.
Under-12yrs Tamariki Vaccination
Getting our under-12yrs tamariki vaccinated is crucial. As of 11 February, tamariki Māori made up 58.5% of all under-12yrs hospitalizations.
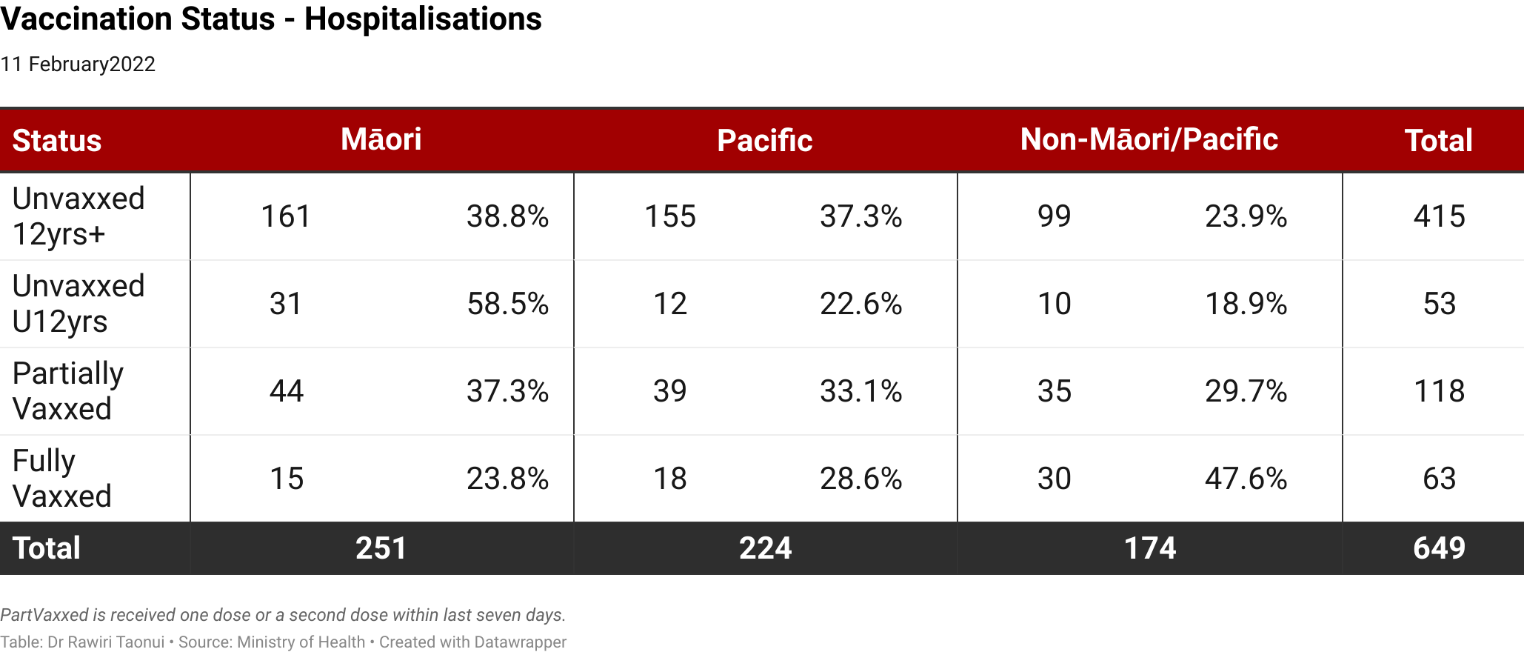
Photo Supplied
The tamariki vaccination rollout is also not working. The Ministry of Health makes much of a consultation and design process.
While there has been consultation, the Ministry has not picked up many of the key requests such as school-located vaccination and appointing a Tamariki Vaccination Monitoring Group.
Consequently, the tamariki Māori equity vaccination gap is huge. The gap is also widening.
The official Health Service User (HSU 2020) figures from the Ministry of Health has a gap of 20.5% between Māori and All Ethnicities. The gap has increased by 2.1% since Waitangi Day,
And the gap is already much larger. Comparing tamariki Māori with non-Māori children and making a conservative adjustment for an undercount in the HSU (2020) compared to the NZ Statistics Estimate of the Resident Population (ERO 2021), reveals an equity gap of 26.4%.
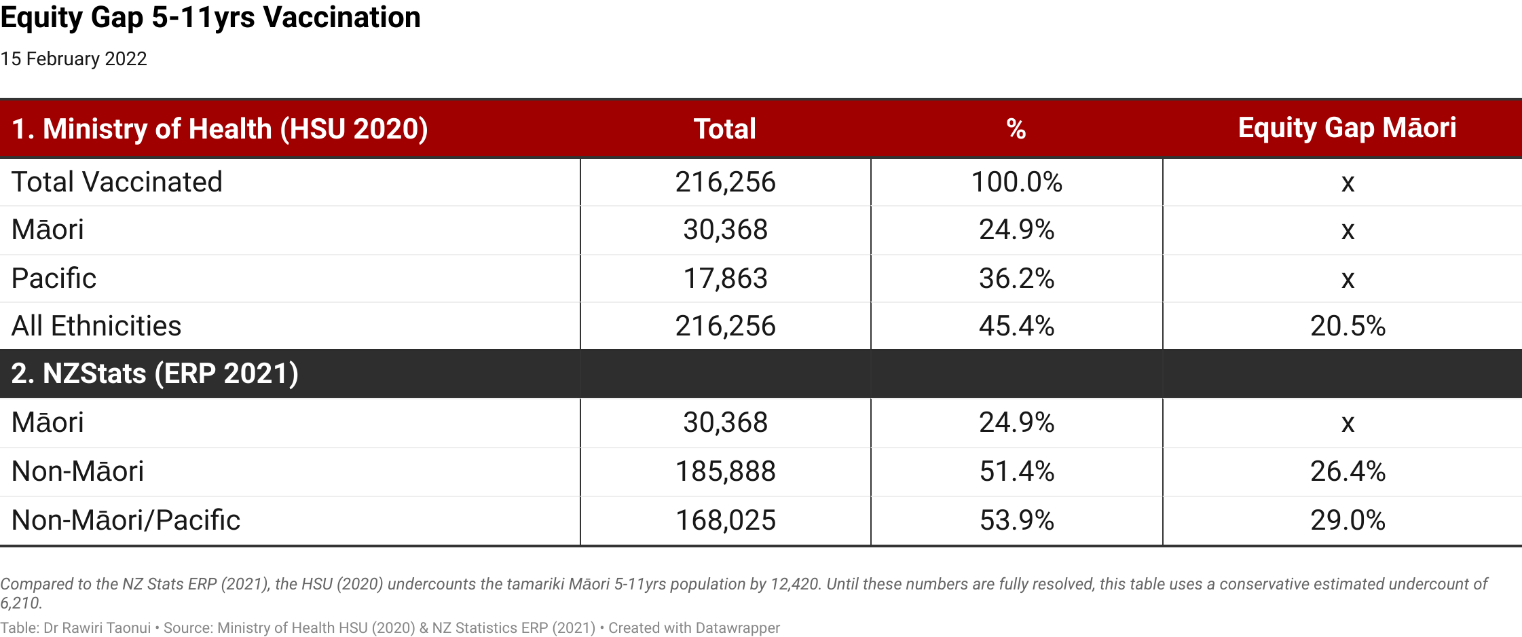
Photo Supplied
Going further and comparing Māori with non-Māori/Pacific shows a very larger gap of 29.0%.
Māori Vaccination
Many in government will blame Māori and anti-vaxxer misinformation for the lower tamariki vaccination rollout. The contrary is closer to the truth. Whānau Ora, iwi, and other Māori health providers have demonstrated significant success when provided with the resources to implement the right strategies.
The original vaccination rollout last year disadvantaged Māori because it did not allow Māori to vaccinate as whānau, the age-band approach pushed the youthful Māori population to the back of the queue, and the Ministry withheld crucial Māori vaccination data for several months. Nevertheless, with additional government resourcing late last year, providers have vaccinated over 112,000 Māori since 1 November. This 27.9% increase is higher than all other ethnicities combined.
Māori Boosters
Ensuring our pakeke receive their booster vaccinations is important. World data shows that over six months, the effectiveness of the second vaccination dose wanes significantly faster against Omicron than the Delta variant. Current research shows that the third booster lifts protection against Omicron and that this protection lasts longer.
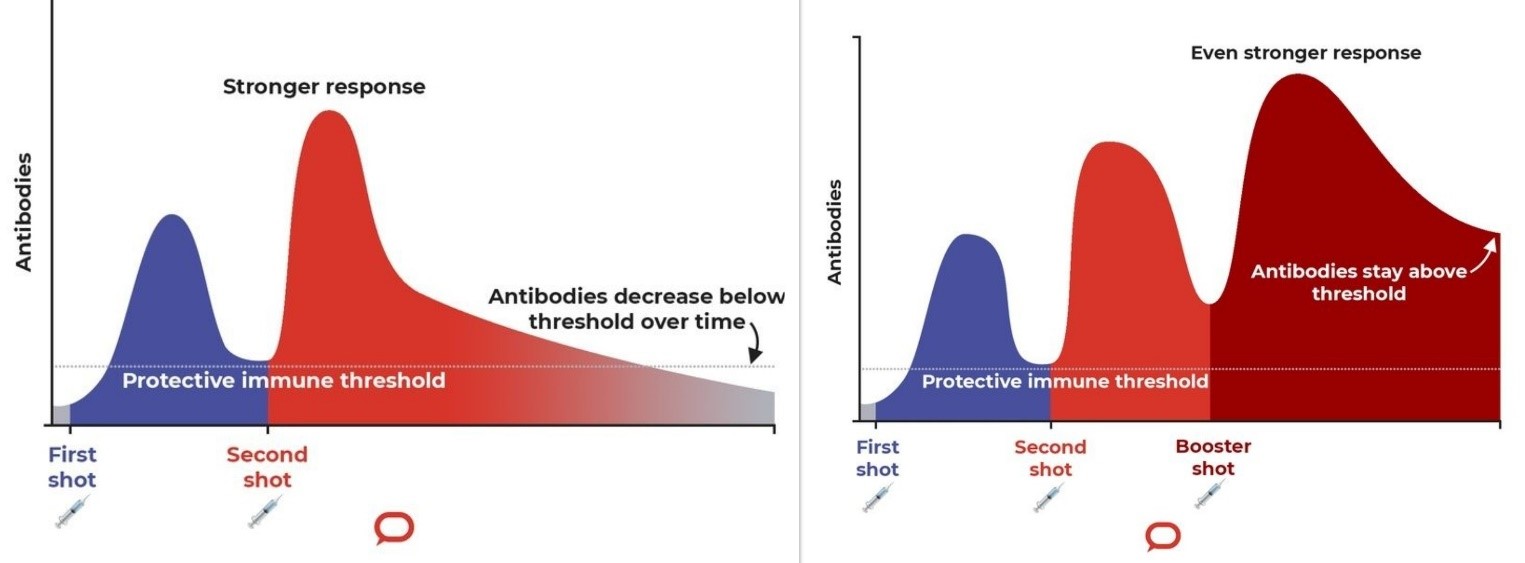
Photo Supplied
The government decision on 4 February, to reduce the waiting period for booster shots has proved vital. Since over 43,000 Māori have obtained boosters, the 37.1% increase higher than the 33.6% for the Pākehā adult community.
Preparation
Whānau Māori and their households, marae, hapū, or other organizations must have plans in place to care for the sick and protect those at risk of infection. This includes gathering food, basic cold-flu type medicines, and medical supplies such as masks and disinfectants.
Many whānau do not have the resources to gather food, basic medicines, and medical supplies sufficient to cover caring for sick family members at home. Those living at distance from primary health care and hospitals face additional risks.
The government has not met calls for a funded Omicron Māori Strategy to support home isolation. With over 6,300 active community cases, home isolation presents a major risk to whānau Māori. We may need to seek help from each other.
The second wave of the Spanish Flu in 1918 took the most lives. After abating, the government sent teams out to check on isolated settlements.
The man who led a party into a kainga in the Waimamaku area in the Hokianga wrote that he found 14 deceased Māori, of which 12 had died. All appeared to have had the Spanish Flu but from the condition of the bodies, he concluded that some had died of starvation because no help had arrived. The only survivors were two young girls. Their mother and four of their brothers and sisters had died. They had lost their father and two siblings during the 1911 Typhoid OutBreak.
In the absence of a government strategy, many of our whānau Māori will fend for themselves. Māoridom has come a long way since 1918. We are in a stronger position than during any other pandemic to look after each other.
Kia noho haumaru, stay safe.
Dr Rawiri Taonui