February 07, 2022
Dr Rawiri Taonui Omicron Māori | Vaccination Equity for Tamariki


The government needs to front foot Māori out of catch-up mode to strengthen a faltering tamariki Māori vaccination rollout.
When Covid-19 first arrived in Aotearoa, the Māori testing regime wavered because the government and District Health Boards (DHBs) failed to properly resource Māori. Once Māori had the resources, they turned the testing around in less than six weeks.
Last year’s age-band centred vaccination rollout failed to allow Māori to vaccinate as whānau and pushed Māoridom’s more youthful population to the back of the queue. In a massive catch-up between September and this year, Māori increased vaccinations by 84.6%, three times the increase for Pākehā over the same period.
We need to do better with the tamariki vaccination rollout.
Omicron and Children
The attitude that Omicron is milder in all cases is ill-founded. Omicron will be milder for most vaccinated persons. According to epidemiologist Rod Jackson, the risk of severe disease and mortality for the unvaccinated is about the same as for other Covid variants.
Children under-12yrs are especially vulnerable since many remain unvaccinated and under-5yrs especially so because vaccination programmes do not yet reach them.
While children are less likely than adults to develop severe illness, they can develop upper-airway problems like croup (inflammation of the voice box and windpipe) and bronchiolitis (inflammation of the lower airway). In rare cases, complications can set in like the life-threatening multisystem inflammatory syndrome (inflammation of the heart, lungs, kidneys, brain, skin, eyes, or gastrointestinal organs). Children can also experience long Covid-19.
Countries across the world are witnessing record numbers of Omicron child hospitalisations. In South Africa, children and teens under-20yrs were 17% of all hospital admissions during the initial Omicron surge compared to 4% during other variant fuelled peaks.
In Europe, child admissions under-9yrs in France are six times greater and under-5yrs hospitalisations in England and Spain three times higher than previous records. In Britain, 117,000 children have long Covid. The United States reported 1.1 million child cases in the week ending 20 January. Under-17yrs hospitalisations are 820 per day across the country. More than 1,000 children have died from Covid.
Indigenous Children
Indigenous children face additional risks because of impoverished living situations and health inequities, particularly in situations with concerns about youth mental health, depression, and suicide. Health structures are also vaccinating Indigenous children at lower rates than non-Indigenous populations.
Unvaccinated Aboriginal children are 40% of all cases in western New South Wales. The Australian data shows that 21.3% of Indigenous children aged 5-11yrs have been vaccinated compared to the national rate of 40%. In Canada, children aged 5-19yrs have the highest Covid infection rates on First Nations reserves.
In New Zealand, tamariki Māori are 53% of all Covid cases and 63% of all hospitalisations under-12yrs. Māori are also behind in the tamariki vaccination rollout.
Tamariki Māori Vaccination
How health authorities present data can obfuscate the extent of the gap between non-Indigenous and Indigenous children. The Ministry of Health (Ministry) website annotates an 18.4% gap between ‘All Ethnicities’ (41.5%) and Māori (23.1%) in the child vaccination rollout.
The 2020 Health Service User (HSU) index the Ministry uses to tabulate vaccinations, counts 115,600 tamariki Māori in the 5-11yrs age group.
This is significantly lower than the 127,980 we can calculate from the NZ Statistics 2021 Estimate of the Resident Population (ERP). This evidences a potential HSU undercount of 12,380.
Separating Māori and non-Māori and applying a conservative undercount of 10,000 shows that the equity gap is a wider 25.8%.
Going a step further and comparing Māori and Pacific peoples with non-Māori/Pacific shows the equity gap for Māori is 28.8%.
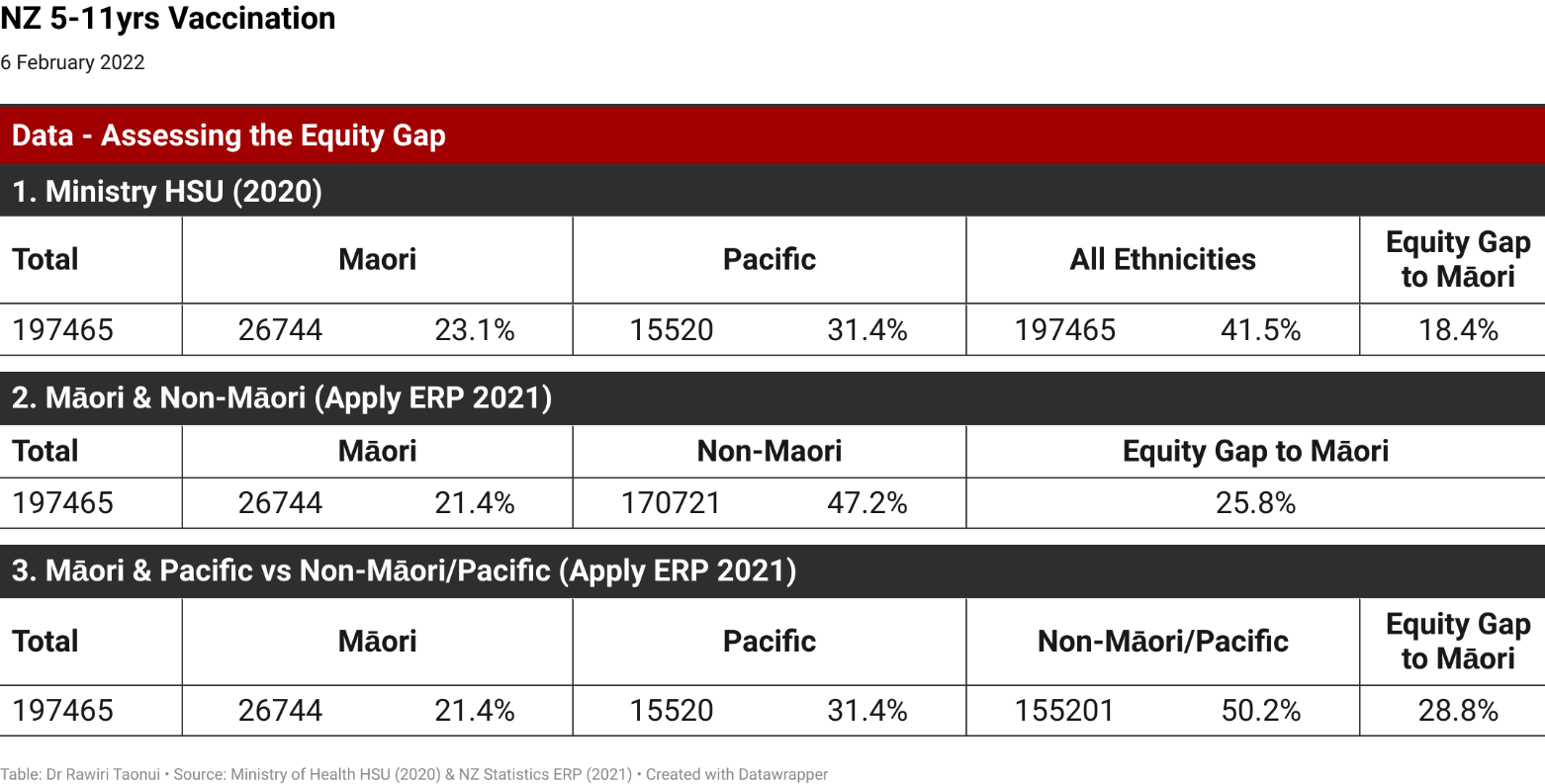
Photo Supplied
Mā te Māori mō te Māori – By Māori for Māori
The willingness of the government to move Māori from catch-up mode and place us on the front foot is what we need to close the equity gap on the tamariki vaccination. There are five main priorities.
• Māori Vaccination Monitoring Group
Last year, a Māori vaccination advisory committee several steps removed from key decision-makers did not work. The government needs to appoint a broadly representative Māori Vaccination Monitoring Group with direct access to data and top officials in the Ministry and Ministers in Cabinet.
This is important to ensure that the government delivers the right support to the best flax roots Mā te Māori Mō te Māori (By Māori For Māori) whānau centred tamariki vaccination strategies so that they can mahia te mahi (do the job). The priority is urgent. On current numbers, we are already in catch-up mode.
• District Health Boards (DHBs)
During the 1913 Smallpox epidemic, it was illegal for a Māori person to administer the vaccine. Last year, one DHB refused to allow qualified nurses and doctors from a Māori provider, the second-largest general practice in their region, to conduct tests. This year, Māori groups report that some DHBs are slow to train and credential Māori vaccinators. This could be a capacity issue. Whatever the cases, the government, Ministry and DHBs should immediately rectify this.
• Schools
In a stunning turnaround from last year, Māori have been less than 10% of 1,500 new cases over the last 10 days. The vector for increasing cases in the Māori community will come as our tamariki return to school and mix with kids from other communities. Vaccinating low decile schools with high tamariki Māori enrolments is the only option to alleviate that vulnerability.
Doing so will come with the risk of harassment from an increasingly emboldened and organised anti-vax opposition. The government needs to support the vaccination of tamariki in schools and follow the example of Canada in establishing ‘bubble’ and ‘safety’ zones around schools, vaccination centres and hospitals to protect against what Canadian leaders term ‘Covidiots.’
• Eight Weeks to Three Weeks
The current wait time for the second tamariki dose is eight weeks. Pfizer-BioNTech, the manufacturer of the vaccine, the US Centres for Disease Control and Prevention (CDC) and Health Canada recommend the tamariki vaccination be given three weeks apart. The government should explore the viability of this advice to lift the protection of our tamariki as expeditiously as possible.
• Data
The Ministry of Health must hand over the data requested by the Whānau Ora Commissioning Agency. The Ministry handed over some data last year but only after two High Court cases and then only a few days before Christmas. Māori are behind in the tamariki vaccination. This is an urgent priority.
Kotahitanga
Māori leaders have stood tall during the pandemic. They carry the welfare of our communities upon their shoulders. Te Whakakaupapa Urutā are our most effective medical advocates. The Whānau Ora Commissioning Agency, our most assiduous street-level operation, took the Ministry to the High Court to obtain vaccination data. The Māori Council took the Crown to the Waitangi Tribunal. Iwi and other leaders have mobilised whole communities.
Some leaders claim an exclusive right to co-design the Māori Covid response. Old iwi versus non-iwi tensions have risen. These undermine the pandemic response. Our leaders need to demonstrate an overarching unity on behalf of the people.
Leading a pandemic is not a competition. The Māori that Covid most impacts are those least connected with iwi, urban groups, marae, hapū, hapori community organisations, te reo and tikanga. They are the poorest, the most marginalised, the young, the incarcerated, and the disabled.
Protecting Tamariki, Whānau and Whakapapa
Overseas experience amongst Indigenous communities shows that many of those who do not trust the government will vaccinate if they understand that is about protecting whakapapa protecting whānau and protecting tamariki. This is our clarion.
Noho haumaru, stay safe.
Dr Rawiri Taonui













